Dosimetry without dosimeters
So, Dr. Zoomie, I know they can do blood tests and stuff to figure out how much radiation exposure someone got. Can you tell me how that works? And are there any other ways to tell radiation dose to a person who didn’t have a dosimeter?
You know, I’ve grappled with this in the past – the first time was when I was in the Navy. The specific process we used was only useful if someone was exposed to a high dose of neutron radiation. In this case, we know that neutron radiation can cause stable atoms to become radioactive – knowing the physics behind this phenomenon, by measuring how radioactivity was induced in a person’s body, we can determine how many neutrons they absorbed and how much neutron dose they received. Our quick-and-dirty technique was to take the person all the way forward (as far from the reactor as possible) and put a radiation detector in their armpit – I can’t remember the exact thumb rule we used, but there was a factor we could multiply that reading by to estimate their neutron dose.
So that’s one way to estimate someone’s radiation dose without using a dosimeter – but there are plenty more.
Blood cells
Blood cells are a reasonably good indicator of radiation exposure because the blood-forming organs are very sensitive to the effects of radiation exposure; blood cell counts go down after a high radiation dose. Unfortunately, it might take days or weeks to see this, so if we want a dose quickly we have to look at cells that will be affected by radiation quickly. Lymphocytes (white blood cells) can help here – a high dose of radiation will cause enough damage to lymphocytes that they start to die within a day or so and the higher the dose, the more quickly (and the more dramatically) the lymphocyte count will drop. This is called lymphocyte depletion and there’s a fairly well-known relationship that can be used to calculate radiation exposure from a plot of how lymphocyte counts drop in the first few days following radiation exposure. This is one reason that blood is one of the first samples taken when a patient is known or suspected of having been exposed to radiation, and a CBC (complete blood cell count) is one of the first tests run.
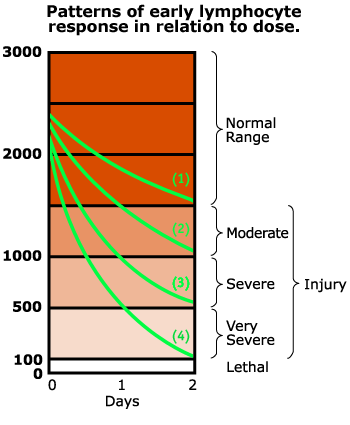
Curves 1-4 correspond roughly to the following whole-body doses:
Curve 1 – 3.1 Gy
Curve 2 – 4.4 Gy
Curve 3 – 5.6 Gy
Curve 4 – 7.1 Gy
Genetic damage
One of the ways radiation harms cells is by damaging the cell’s chromosomes; in particularly, radiation exposure can cause normally X-shaped chromosomes (the point at which the two strands cross is called the “centromere”) to cross twice, forming what’s called a “dicentric” chromosome that our cells have problems with transcribing to form the proteins that keep our bodies running. One or two dicentric chromosomes are almost always going to be present if we look hard enough, but if the number we count is high enough then we know that there are enough “extra” dicentrics to confirm a high radiation exposure; if we check enough cells and see enough of these extra dicentrics then we can start to use them to determine what that dose was.
One of my former colleagues in the early 1990s had a high dosimeter reading – over 50 rem – and the Radiation Safety Officer needed to find out if this dose was real, if the dosimeter had malfunctioned or been misread, if the reading had been falsified, or something else. So the RSO ordered the worker to have a blood sample drawn, which was sent to one of the handful of labs in the world (at that time) to be analyzed for dicentric chromosomes. When the results came back they showed a dose of less than 5 rem (the lowest dose that techniques at that time could quantify), telling us that the worker had not received a dose of 50 rem and had very likely not exceeded his annual dose limit. To get a better idea of his exposure we had to do a dose reconstruction.
Dose reconstruction
In the case I mentioned above we knew that the worker didn’t get the high dose of 50 rem and likely didn’t exceed a dose limit. But if the RSO took the conservative path and assigned a dose of 5 rem then the guy wouldn’t be able to do any work with radioactivity for almost 5 months – a lot longer than the RSO wanted. So we needed to investigate to try to come up with a reasonable dose that could be entered into his dosimetry records. We actually used several methods – here are some of them.
Comparisons with previous months: We dug out monthly dosimetry records for this employee for the previous year; his highest exposure in any one month was 20 mrem and the average exposure was 15 mrem monthly. His workload in the month he received the high reading was similar to that of the other months.
Comparison with coworkers: None of the other radiation workers had received more than 30 mrem in any single month over the previous years and they averaged about 10 mrem monthly during this period.
Measuring dose rates in areas where he worked: This worker spent time working with nuclear medicine and radiation oncology patients and he was also responsible for managing the radioactive waste and sealed source inventory and leak test programs. We measured radiation dose rates in all of the areas where he’d worked that month, none of which exceeded 5 mR/hr in accessible areas.
Dose calculations: Using his work logs and the radiation dose rates we’d measured we were able to calculate the dose he likely received during his work in each of those rooms using various assumptions about the length of time and his exact location in each room. The highest calculated dose was about 100 mR and the lowest was about 10 mR.
These estimates made it clear that he could not have received the dose shown in the dosimetry report. The RSO wrote up the methodology and results of each and assigned a dose of 100 mrem (the highest calculated) and sent the report to the regulators and the dosimetry vendor.
Symptoms
Health effects that occur following a short exposure to high or very high dose rates are called deterministic health effects; they’re called this because, once a certain dose is exceeded, these health effects are going to appear. Radiation sickness, for example, won’t appear at a whole-body radiation dose of less than 70 rem and they’re certain to occur above a dose of about 100 rem, so if a person doesn’t get sick then we know that they didn’t receive more than 100 rem of dose. Skin burns require a dose of at least 600 rem to the skin that develops the burns (but hair loss requires only 300 rem) – these various thresholds can be used to determine the maximum or minimum radiation exposure a person, or the affected part of a person, likely received.
Another symptom that can be useful is the time to emesis – the amount of time between when a person was exposed to a burst of radiation and the time they begin vomiting from radiation sickness. According to the International Atomic Energy Agency (IAEA), a person who begins vomiting within 10 minutes of receiving a high radiation exposure likely received more than 800 rem and will almost certainly die from radiation sickness, while someone who doesn’t begin vomiting for more than 2 hours almost certainly received a survivable dose (less than 200 rem). Intervals of intermediate duration suggest intermediate doses. Using any of a number of deterministic effects, we can develop reasonably accurate dose estimates for those exposed to very high levels of radiation exposure.
Electron spin resonance (also Electron paramagnetic resonance)
This is a biodosimetry method that, to be frank, I just don’t understand all that well. What I do know is that tooth enamel can be examined…somehow…to determine the total amount of radiation to which it has been exposed. And it requires pulling a tooth.
Summary
As we’ve seen, there are a number of different ways to determine how much radiation a person has been exposed to. Some require samples (e.g. blood, teeth), some require calculations (e.g. dose reconstruction), some are largely administrative (e.g. comparing doses to the person exposed or to their colleagues) – but they are all accepted methods to try to determine how much radiation a person was exposed to…whatever it was they were doing that got them exposed.
This is a brief summary – if this has just whetted your appetite, check out this paper that’s free online – it’s got a lot of great information and it’s largely aimed at people who don’t do this for a living.
